Tips on angioplasty for chronic total occlusion (CTO)
Tips on angioplasty for chronic total occlusion (CTO)
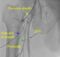
Tips on angioplasty for chronic total occlusion (CTO): Micro vessels are there in about forty percent of the chronic total occlusions. CTOs can have a proximal cap and a hard plaque. Use penetration technique to cross the cap. Other techniques are probing technique and controlled drill. Contralateral coronary injection taken from the outset itself will be good to assess the missing segment and the distal track in CTO.
CT angio may help in visualizing calcification and microchannels while planning PCI. CT angio can also serve as a roadmap and can show the calcification in the missing segment in case of CTO. If calcium score is more than 700 Hounsfield units, the chance of success is low.
Make only 1-2 mm tip curve while crossing a CTO while you can use a 2-3 mm tip curve for negotiating a stenosis. Use hydrophobic wires when there are side branches as hydrophilic wires tend to slip into the side branches easily.
CTO guidewires have a tip which has more than 3 grams strength while floppy wires have less than one gram load strength. The tip of the wire could be hydrophobic or hydrophilic. Wires can have tapered and non tapered tips. Hydrophilic wires are more likely to perforate. Tapered wires can go into small microvessels. Stiff wires can be used for in stent restenosis as vessel outline is marked by the stent.
The first wire might cross only in one out of six cases of CTO. Escalate the wire if the initial wire is not crossing. Over the wire micro catheters help in crossing tough lesions, but tips of hard wires may perforate. Exchange a harder wire for a softer wire after crossing, before stenting as it will prevent perforation. Wire exchange can be done with the micro catheter in situ.
Pulling back a subintimal wire can cause catheter induced proximal dissection at the ostium. This is more likely in a calcific lesion. This ostial dissection can also extend into the aorta. When it is seen that a wire has gone subintimally, it is better to keep it there as a marker and use another wire to cross the lesion (parallel wire technique). In parallel wire technique, use a stiffer second wire and the tip can be shaped differently to enter the true lumen.
Vessel may look smaller after ballooning. Give intra coronary nitroglycerine before stenting to assess the size to avoid stent under sizing.
It is ideal to have 7F or 8F guide catheters for CTO procedures to take extra balloons and wires. The guide catheter should be able to withstand prolonged exposure to blood at 37 degrees Centigrade. Extra back up guide catheters are preferred for CTO interventions. Do keep in mind that stiffer catheters are also more traumatic. For using a left Amplatz catheter in the right coronary artery (RCA), a large roomy RCA is needed, or else it can dissect. Prior to finally removing the guide wire after the procedure, back out the guide catheter a little and check the ostium to exclude dissection.
Ikari catheter which gets support from the opposite aortic wall is a good option for RCA with an anomalous origin.
4F catheters can be pushed into anomalous left circumflex (LCX) right across the lesion without traumatising the rest of the proximal vessel. It is useful when other catheters won’t get engaged well. 4F catheters may require extreme deep throating when stents do not track into the LCX.
Anchor balloons are useful in CTO interventions. Co-axial over the wire (OTW) balloons can be used in the parent vessel and non co-axial balloons can be used in the side branch. If an ancho balloon in the side branch slips, use a longer balloon. Another technique is to use a third wire in the side branch to prevent slipping of the anchor balloon.
Guide support can be improved by using an additional smaller catheter. A 5F catheter can be introduced into a 7F catheter using a hemostatic valve (mother and child system). Deep throat the 5F catheter about 2 centimeters into the coronary artery so that improved support is obtained.